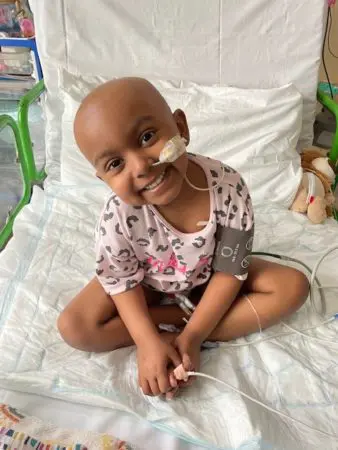
Esha’s story: ‘There’s no way to explain that sinking feeling’
Esha’s parents took her to the GP when she started to feel lethargic and they noticed her toilet habits had changed – they were referred to their local hospital for a blood test and after being told they would hear in a couple of weeks, they got a call within the hour to say they needed to come back immediately as they suspected leukaemia. By the next day Esha was at GOSH having a Hickman line put in and was on chemo the following day.
Diagnosis
“It was probably around late April last year, early May, she started to feel lethargic, more than anything else her toilet habits had changed significantly. We went to the GP assuming she had developed some sort of food intolerance. The GP suggested Esha has a blood test so we had that scheduled and we took her to the local hospital and we were told we would have results back in a couple of weeks. We got home and an hour later I had a call from the hospital saying ‘you need to bring her back immediately’, which is where we learnt she had some form of leukaemia.
“Once we got to GOSH and we did more detailed testing the feedback we got was that it was quite at an advanced stage which is probably why it was picked up quite quickly at blood labs
“There is no real way to explain that sinking feeling when you get told your 4 year old daughter’s got cancer. I just refused that something like that could happen and just dismissed it. Deep down you never really think it would happen to you until it does happen – you don’t really expect it to happen to you.”
Once Esha was transferred to Great Ormond Street Hospital, she had various tests before starting treatment.
Starting treatment
“The following day she had to go through a series of surgical procedures like the bone marrow aspiration, they also had to put in a Hickman line. Then within another day or so it was straight onto chemotherapy so it all moved within three or four days.
“As a four year old you can’t really explain it, I think for her it was very traumatic because until they put the Hickman line in all the blood tests – and she obviously had quite a few – were needles into her veins and that’s a painful experience. I think she had close to 20 in the first 24 hours so it was very traumatic not only for her but also for us because I had to physically pin her down whilst they did that so it was a very unpleasant experience.”
Esha then started chemotherapy treatment, she was put on a plan that would mean having three or four cycles of chemo.
“It was quite strong treatment so within 24 hours or so you see the side effects – the constant vomiting, diarrhoea, hair loss, it happens very quickly and continuously. She finished the first cycle and as part of the first cycle we were offered to go on a clinical trial which we took and what that meant was she got randomised for different doses of drugs but it also meant her results got sent to a national laboratory which has more comprehensive means of doing tests. We went through the first cycle of chemo at GOSH we were told it looked like it was in the right direction, continued with the second cycle of chemo and same message that it looked good based on the tests they could do in the GOSH labs.
“We were about to start the third cycle of chemo when we got a call and got told that the results from the GOSH labs weren’t necessarily comprehensive and the national labs were showing that she was not responding to chemotherapy so that was almost like being told you’d been diagnosed again because we’d gone through cycles and she was heading towards remission only to be told it hadn’t worked”
Esha then had to have a bone marrow transplant, which meant moving to an isolated ward for months to have the transplant. She had the transplant in October 2021 and left hospital four months later in early 2022.
Post-treatment
Despite being home, Esha still requires lots of care.
“Even though she’s home she has full-time care, she has 30+ medications a day, she still has a line for the bloods, she still has a nasal and gastric tube in and the bulk of her calories are through that including all the medications. Transplants kill of your immune system so that can take up to two years to fully recover your immune system so even though we’re home we’re in a bubble so no visitors, we don’t go anywhere, very sterile environments. Our day starts at 4 in the morning and finishes at midnight, that’s the cycle of medications and feeds. Even though we’re home, it’s very hard work and quite draining.”
Paul’s House
During treatment, Esha’s parents would take it in turns to be by her bedside so someone was with her 24 hours a day, seven days a week. They stayed at Paul’s House, Young Lives vs Cancer’s Home from Home in London, which helped them keep Esha safe from infection.
“It was always two [adults] during the day but only one at night. One of us then had to commute back home at the end of the day and come back early in the morning and I think that’s where Young Lives vs Cancer helped, especially when she went into the bone marrow transplant ward. We didn’t want to risk going on the underground, it’s probably one of the worst places to be in terms of infection so we were able to secure accommodation at Paul’s House which was a lifesaver for us.”
Being able to stay at Paul’s House meant Esha’s parents didn’t have to endure the tiring travel to and from the hospital, as well as saving money on the cost of fuel and accommodation.
“One option was looking at temporary short-term rentals but it’s not affordable in that area, it’s ridiculous. Then the other option would have been having to drive in and out [of London] which would mean leaving very late at night and in the morning having to leave around five o’clock just to avoid all the London rush hour, so it would have been very draining, very expensive.
“Paul’s House is amazing. It’s literally a 15-minute walk from the hospital and we didn’t want to be hopping on public transport and that provided that opportunity, something so close, so convenient. We didn’t really know what to expect in terms of standards of living conditions but I was so amazed by how neat and clean and organised it was. Paul’s House is three London townhouses joined together and each with its own kitchen. Because of Covid, you had your own area for cutlery, utensils and food stuff even in the fridges. The other thing we were really dependent on was having a dedicated bathroom – from an infection control perspective – and they were able to provide us that. In terms of having free accommodation in such a central location in London it ticked all the boxes, there was no scenario where it fell short.”
Young Lives vs Cancer social worker
Esha’s family were also supported by a Young Lives vs Cancer social worker who helped them navigate the practical, financial and emotional impact of a childhood cancer diagnosis too.
“Unless you experience cancer first-hand I think it’s hard to explain how hard it can be mentally, physically, emotionally, financially – there are so many things to deal with and it’s just so easy to break and it’s obviously much harder when it’s your child. The volume of information that gets thrown at you, it’s overwhelming – to be able to process that and make decisions is hard in itself and I think having Young Lives providing that help to sort out some of the non-medical help, it was almost like having somebody there to sort it out for you.”
An update on Esha (2025)
Esha went home in February 2022 and is now approaching four years since her transplant. While treatment-related complications and after-effects are still part of her daily life, her dad says she carries on being her bubbly, chatty self.
Her family are sharing their story as part of our 2025 winter campaign, to help more families facing cancer stay together at a Home from Home this winter.
Posted on Thursday 15 September 2022